Home > Dispatches > Daily Dispatches 2016 >Daily Dispatch #14
For the past ten years or so, I’ve had intermittent bloody noses. I do not know what causes this. It might be hay mold, it might be dryness. All the doctors have ever said (during my routine physical) is “Don’t worry.” But I do worry – one of my biggest fears being that I might sometime have a nose bleed and the blood flow won’t stop, meaning that I’ll bleed to death. I have had these nosebleeds for ten years now and never once has the blood flow been excessive. Yesterday in Anatomy and Physiology II – right before lecture, a few drips fell on my lecture notes. I well knew the drill. I took a piece of crumbled tissue and wiped them away, then wiped my nose. Next, I put my middle finger on |
|
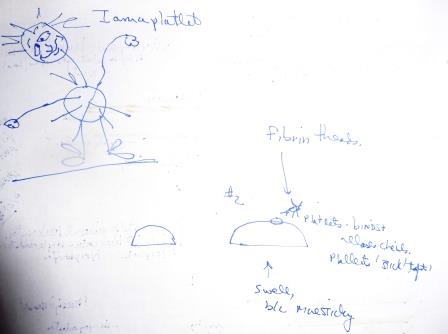
| the firm part of my nose and the pointer finger underneath, and held them there. I then took a few deep breaths. Those sitting on each side of me saw what was going on and then busied themselves. I read the cartoon balloons above their heads – they both read “crazy older woman who is taking this class is having a nose bleed. Avoid, avoid.” I have an acquaintance who claims there are no coincidences. Sometimes, ya gotta wonder, and this was one of those times. I mean, what was the day’s anatomy and physiology lecture topic? You got it – the blood and clotting. I kid you not. It was not the information in the previous chapter, that is the endocrine system, nor was the information in the next chapter, that is the circulatory system. No, it was The Blood. So there I sat as class began and Dr. Nevis strode to the podium. Half of my thoughts were focused on my condition and the other half were focused on the lecture material. Clotting and coagulation isn’t something that’s easy to comprehend, but in retracing my steps, I might better understand the basics. Dr. Nevis began this portion of the lecture by providing us all with a definition of hemostasis – it is the first series of reactions involved in stopping bleeding. Hemostasis requires clotting factors, and as well, substances released by platelets and injured tissues. There are three steps, or stages involved in clotting, the first being vascular spasm. This, defined, is the vasoconstriction of damaged blood vessels. Vasoconstriction is most effective in smaller blood vessels. Triggers for vasoconstriction are direct injury to vascular smooth muscle, chemical release by endothelial cells and platelets, and pain reflexes. Endothelial cells are cells that line the INSIDE of blood vessels. The second trigger is Platelet Blood Formation. What happens is that 1. the damaged endothelium exposes collagen fibers. 2. The platelets stick to collagen fibers, swell, become spiked and sticky, and then release (ta da) chemical messengers. ADP causes more platelets to stick and release their content. Serotonin and thromboxane A also enhance vascular spasm and platelet aggregation. Then finally, there is coagulation. In this stage of the process, the platelet plug is reinforced with fibrin threads. Also, blood is transformed from a liquid to a gel. There are then a series of reactions involving clotting factors, which are called procoagulants. I took a close look at the droplets of blood on my tissue. They were drying out – I suspect that the watery substances, maybe plasma, had been absorbed by the tissue, leaving the cells embedded in the material. I do not know – I will ask Dr. Nevis. I then looked up and nudged the guy next to me, pointed to the tissue and whispered “blood.” He nodded, and then went back to taking notes. A good thing, I think, that he was concentrating on the understanding the theory behind hemostasis. It was at this point in the lecture that things got – complicated. This is always the case with anatomy and physiology. For me, the more minute details of physiology are difficult to understand. So, here a very basic summation of the three phases of coagulation. In the first phase, Prothrombin activator is formed. In the second phase, the Prothrombin activator converts Prothrombin to the enzyme Thrombin. And in the third phase Thrombin catalyzes Fibrogen to fibrin. And there you have it, all systems then return to normal, meaning, there is no more blood loss. Then once you have a clot, other things happen. You have clot retraction which stabilizes the clot. The actin and myosin in the platelets contract in 30-60 minutes. This contraction pulls on the fibrin stands, squeezing serum from the clot. This then draws the vessel edges together. Vessel repair follows. Even as clot retraction is occurring, the vessel is healing. Furthermore, platelet-derived growth factor (PDGF) stimulates division of smooth muscle cells and fibroblasts to build blood vessel walls. And additionally vascular endothelial growth factor (VEGF) stimulates endothelial cells to multiply and restore the endothelial lining. I further learned that there are disorders of hemostasis – one being thromboembolic disorders, or undesirable clot formation and the other being bleeding disorders, or abnormalities that prevent normal clot formation, like hemophilia. All righty. This part of the lecture was about over. I stuffed my tissue in my jeans pocket and felt inside my nostril with thumb and forefinger. Dark granules fell onto the page before me. Clotting – it had occurred and healing was taking place. A little knowledge is a good thing. In this particular instance, I realized that as far as my nose goes, all systems are go. I do not know why the blood vessel (every so often) ruptures – but I am a tad bit less fearful about the prospect of my hemorrhaging and dying a gosh darn bloody death. Most importantly – I realized as I was leaving class that I had something to write about. I could, if I so chose, draw upon an assertion of John Dewey, the renowned educator and author of Experience and Education. Dewey said that learning best occurs when we make connections. In this particular instance, I made the connection between what was happening to me physiologically, and what, coincidently, was about the very same subject, that is blood clotting. |
|